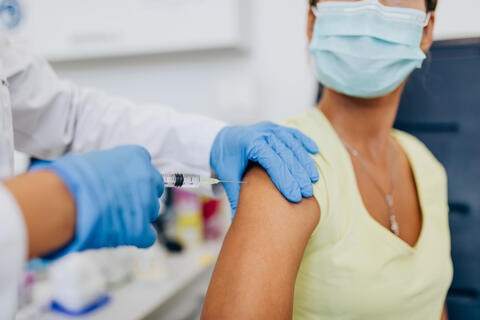
The message from health chiefs is clear: Covid-19 vaccines are safe for pregnant women. While a question mark hung over this vital detail earlier on in jab trials, today there is clear data to show there is no risk to mothers-to-be or their unborn children.
It is a major step forwards in the battle against the virus.
And there is even evidence that vaccinating women now may have knock-on benefits for any children they have in the future, too. Since the immunity provided by a Covid vaccine is passed down to the foetus, wide take-up of the jab will eventually lead to a generation of children with in-built resistance.
While the risk that Covid poses to pregnant women and babies is generally low, studies have shown that women who catch it while pregnant are two to three times more likely to give birth prematurely – which can endanger the newborn. However, the jab dramatically reduces this risk.
Two other studies have also shown that vaccinated mothers pass more protective SARS-CoV-2 antibodies on to their newborns than mothers who had COVID-19 while pregnant. https://t.co/oVvLLo2eAz
— National Geographic Magazine (@NatGeoMag) May 7, 2021
Despite this, experts say that roughly one in five pregnant patients are hesitant about getting a Covid jab. Other studies suggest this is likely to be higher – the results of a poll of more than 1,000 pregnant women, reported last week, showed at least one in three weren’t sure they’d have one.
‘The majority of pregnant women understand it is important, but some say they aren’t sure they want to take anything while pregnant,’ says Dr Pat O’Brien, vice-president of the Royal College of Obstetricians and Gynaecologists.
Yet scientists remain adamant there is no evidence to suggest any of the Covid vaccines have any effect on pregnancy.
One leading scientist told this newspaper that having the vaccine was the ‘best thing you can do for your baby’ due to the reduction in risk of a premature birth. So why all the worry?
Some say the seed of doubt was planted even before the beginning of the vaccine programme.
In November, Pfizer became the first company to announce that its vaccine was effective against Covid-19 – but the company also said it hadn’t yet been tested on pregnant women.
This is entirely normal for vaccine trials, says Dr O’Brien, adding: ‘Traditionally, pregnant women are excluded from these studies as a precaution.’
Early studies of the vaccine on animals also showed no issues around pregnancy. Nonetheless, due to a lack of data, the Government warned expectant women not to have the jab – NHS leaflets circulated at the start of the rollout reiterated this. The effect, experts say, was to entrench worries in a group already naturally cautious about what medicines they take.
Meanwhile, other countries were taking a different approach.
Israel, the world leaders in vaccinations, went as far as to prioritise pregnant women for a vaccine, while the US decided they would be vaccinated in early December.
Those involved in the decision to delay in the UK stand by it.
Vaccines have been available 5 months. Pregnancy lasts 9 months! I am not anti-vax, I have had 2 jabs. How can we possibly know yet if vaccines are safe for pregnant mothers and their babies? https://t.co/blFv7hSHwm
— Anthony Hinton ? (@TonyHinton2016) May 9, 2021
Professor Adam Finn, a member of the Joint Committee on Vaccination and Immunisation (JCVI), the advisory group which guided the UK’s vaccine rollout, says there were concerns that approving any vaccine before there was clear evidence of safety would put off pregnant women.
He says: ‘Everything that we know about vaccines pointed to these ones being safe for pregnant women, but that’s not enough to go on, you need data.
‘If we’d come out and said we assume these vaccines are safe, but expectant mothers should make up their own minds, I’m not sure that would have gone down well. We had to come up with evidence which showed the vaccines were safe for mother and baby. You could argue that, for this reason, the American approach was a bit rash because they decided to move ahead before that evidence appeared.’
Instead, the JCVI decided to wait for data from America to filter through before making a call.
In early April, that data arrived in the form of a major study published by the US Centers for Disease Control and Prevention (CDC). It had tracked the condition of more than 90,000 pregnant women who had received a vaccine, the majority of them in their third trimester.
The CDC was able to report that there were no safety concerns.
Since then, the number of pregnant American women who have had a vaccine has risen to more than 105,000. However, finer data released from within that study set off fresh anxieties.
The CDC closely monitored more than 800 participants. Of that group, 712 had a live birth, while 115 suffered a loss of pregnancy.
This means that roughly one in eight woman who’d been jabbed had lost their baby.
It is a scary thought but, in fact, this is identical to the average rate of pregnancy loss in the population, according to NHS figures.
Armed with this knowledge, on April 16 the JCVI made the recommendation to the Government that pregnant women, along with any planning pregnancy or currently breastfeeding, should be invited for vaccination along with their age and clinical risk group.
However, the recommendation extended only to the Pfizer and Moderna jabs. It did not include the UK’s Oxford-AstraZeneca vaccine.
Confidence in the AstraZeneca vaccine has fallen in recent weeks in the UK following reports it could cause rare blood clots. Experts maintain the decision to not give pregnant woman the AstraZeneca jab is unrelated to this. Instead, they say it is because of a lack of jab-specific data.
‘There’s nothing to suggest AstraZeneca would be unsafe for pregnant women,’ says Prof Finn, ‘but without the data we can’t make that call just yet.’
Another area of worry has been the possibility that Covid vaccines could effect fertility.
According to the Office for National Statistics, young women are one of the most vaccine-hesitant groups in the country, in part because of worries about becoming pregnant in the future. But experts are clear there is no foundation to these worries.
Dr O’Brien says: ‘In recent months there’s been a big surge of anxiety about infertility. It’s hard to know where it’s come from, because there is absolutely no evidence to suggest these vaccines would affect fertility.’
Scientists point out that there is no biologically plausible mechanism by which vaccines, for Covid or for any other disease, could lead to infertility and there has never been any evidence of vaccines in the UK causing infertility.
While it is not entirely clear where the infertility theory has come from, several reports have pointed to conspiracy videos shared on Facebook and YouTube.
With the under-40s expected to begin getting invitations to be vaccinated in the coming weeks, the Government will soon know the full extent to which pregnant women – who statistically are more likely to be in this age bracket – are willing to come forward.
Despite early misgivings, Dr O’Brien is confident uptake will be high: ‘Women were waiting for assurance. Now they have it.’
This article has been adapted from its original source.